Geriatric dentistry
Geriatric dentistry focuses on the oral health of elderly patients, who often have complex medical histories and take multiple medications. In addition, they may have psychological and socioeconomic problems that require sophisticated dental management. A key principle of geriatric dentistry is that elderly patients often experience different symptoms of dental decay and gum disease than younger patients. As a result, dental treatment for the elderly is tailored to any physical and mental limitations they may have.
The elderly are more susceptible to poor oral health, which can lead to a loss of appetite, malnutrition, and various metabolic disorders. In extreme cases, poor oral health can lead to depression. There is a strong link between periodontal disease and other illnesses such as heart disease, stroke, diabetes, and osteoporosis. With the number of elderly persons of advanced age (85 years or older) with mental disorders such as Alzheimer disease reaching epidemic proportions, dental management of affected individuals has become a major challenge in clinical dental practice. The elderly often take many medications, which have adverse side effects such as dry mouth, a major cause of dental decay. The effects of aging result in changes in lip posture, chewing efficiency, and ability to swallow and taste and in an increase in diseases of the hard and soft tissues of the mouth.
The elderly population faces significant oral health problems, including dental decay, periodontal disease, and tooth loss. This backlog of oral disorders demands education, research, and advanced clinical training in geriatric dentistry.
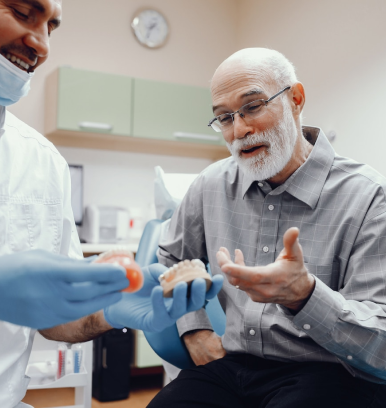
What exactly is geriatric mobile dentistry?
It is a branch of dentistry that deals with the provision of dental care to elderly people in their homes or other long-term care facilities. It aims to improve the quality of life of geriatric dental patients by providing them with the necessary dental treatments and preventive measures.
What leads seniors to suffer from poor oral health?
A recent survey suggests that a sizable percentage of seniors in the US do not have regular access to dental care. This can be due to a few factors, such as lack of transportation, financial constraints, or simply not being able to find a dental office that is convenient for them. As a result, many seniors suffer from poor oral health, which can lead to a decrease in their quality of life.
How can mobile dentistry help geriatric patients?
Geriatric mobile dentistry helps to improve the oral health of seniors and improve their quality of life. This type of dentistry brings dental care to the patient, instead of the patient having to travel to a dental office.
What are the oral problems that can be addressed through geriatric mobile dentistry?
The most common oral problems that are seen in seniors are tooth decay, gum disease, and missing teeth. These problems can lead to a decrease in the quality of life, as they can make it difficult to eat the foods we enjoy or gum disease.
Geriatric mobile dentistry can provide a wide range of services to improve the oral health of seniors. These services can include teeth cleaning, cavity fillings, denture fabrication and denture repairs. This type of dentistry can also provide education on proper oral hygiene, which can help to prevent future problems.
If you are a senior and are suffering from poor oral health, consider contacting a geriatric mobile dentist to see how they can help improve your quality of life.
What should elderly patients do in a dental emergency?
There are a few things that you can do in order to ensure that your elderly patient is well taken care of in case of an emergency:
It is important that you have a list of emergency contacts for your elderly patient. This should include their primary care physician, as well as any other specialists that they see on a regular basis. You should also have the contact information for their family members or close friends who can be reached in case of an emergency.
You should make sure that your elderly patient has a plan in place in case of an emergency. This plan should include what steps to take in order to get to the hospital, as well as what to do once they are there. It is also important to have a list of medications that your elderly patient is taking, as well as any allergies that they may have.
You should make sure that you are familiar with the symptoms of a dental emergency. This way, you will be able to recognize the signs and symptoms of an emergency and take the appropriate steps to help your patient.
You should always have a first aid kit on hand in case of an emergency. This kit should include items such as gauze, gloves, and antiseptic wipes.
You should make sure that you know how to properly handle a dental emergency. This includes knowing how to properly clean the area around the tooth, as well as how to apply pressure to the tooth in order to stop the bleeding.
You should make sure that you are familiar with the symptoms of a stroke. This way, you will be prepared and take the appropriate steps to help your patient.
You should make sure that you are familiar with the symptoms of a heart attack. This way, you will be prepared and take the appropriate steps to help your patient.
You should make sure that you are familiar with the symptoms of a seizure. This way, you will be able to recognize the signs and symptoms of a seizure and take the appropriate steps to help your patient.
You should make sure that you are familiar with the symptoms of an allergic reaction. This way, you will be able to recognize the signs and symptoms of an allergic reaction and take the appropriate steps to help your patient.
You should make sure that you are familiar with the symptoms of a diabetic emergency. This way, you will be able to recognize the signs and symptoms of a diabetic emergency and take the appropriate steps to help your patient.
If you or your loved one is ever in a situation where you are not sure what to do, it is always best to err on the side of caution and call 911. This way, you can get the help that you need in order to ensure that your patient is well taken care of.
Darkened teeth
Teeth may become darkened due to changes in dentin, which is the bone-like tissue that lies beneath tooth enamel, as well as from consuming staining foods and drinks over time. Another cause of darkened teeth is thinning of the outer enamel layer, which allows the darker yellow dentin to show through. If you have one or more darkened teeth, it may be a sign of a more serious issue and you should see your dentist.
Dry mouth
Dry mouth is caused by a reduction in saliva flow, which can be a side effect of cancer treatments that use radiation to the head and neck area, as well as certain diseases such as Sjögren's syndrome. Many medicines can also cause dry mouth.
Diminishes of taste
The sense of taste diminishes as people age, but diseases, medications and dentures can also affect this sense.
Root decay
This is caused by exposure of the tooth root to decay-causing acids. The tooth roots become exposed as gum tissue recedes from the tooth.
Gum disease
Gum disease is caused by plaque and can be made worse by food left in teeth, use of tobacco products, poor-fitting bridges and dentures, poor diets, and certain diseases, such as anemia, cancer, and diabetes. This is often a problem for older adults.
Tooth loss
Gum disease is one of the main reasons why people lose their teeth.
Uneven jawbone
An uneven jawbone can be caused by missing teeth, which allows the rest of the teeth to drift and shift into open spaces.
Denture-induced stomatitis
This condition is caused by ill-fitting dentures, poor dental hygiene, or a buildup of the fungus Candida albicans. It is characterized by inflammation of the tissue underlying a denture.
Thrush
A weakened immune system can cause an overgrowth of the fungus Candida albicans in the mouth, leading to thrush. While age is not the only factor in oral health, it can be a dominant factor in certain medical conditions, such as arthritis in the hands and fingers, which make brushing or flossing teeth difficult to impossible to perform. Drugs can also affect oral health and may make a change in your dental treatment necessary.
Oral Hygiene Tips for Seniors
Good oral hygiene is essential for seniors to maintain their natural teeth. If oral hygiene is neglected, plaque can build up quickly on seniors' teeth, which can lead to tooth decay and gum disease.
To maintain good oral health, it's important for all individuals -- regardless of age -- to:
-
Brush at least twice a day with a fluoride-containing toothpaste
-
Floss at least once a day
-
Rinse with an antiseptic mouthwash once or twice a day
-
Visit your dentist on a regular schedule for cleaning and an oral exam
According to the American Dental Association, antibacterial mouth rinse can reduce bacteria that cause plaque and gum disease.
What Seniors Can Expect During a Dental Exam
If you're a senior headed for a check up, your dentist should conduct a thorough history and dental exam. Questions asked during a dental history should include:
The approximate date of your last dental visit and reason for the visit
-
If you have noticed any recent changes in your mouth
-
If you have noticed any loose or sensitive teeth
-
If you have noticed any difficulty tasting, chewing, or swallowing
-
If you have any pain, discomfort, sores, or bleeding in your mouth
-
If you have noticed any lumps, bumps, or swellings in your mouth
Your dentist will examine your face and neck for any skin discoloration, moles, or sores. They will also check your bite to see if there are any problems with how your teeth come together when you open and close your mouth. Additionally, they will examine your jaw for any signs of clicking or popping in the temporomandibular joint. They will also check your lymph nodes and salivary glands for any sign of swelling or lumps. Finally, they will examine your inner cheeks for any infections, ulcers, or traumatic injuries.
Your dentist will ask a few questions about when you wear your dentures or other appliances, and will also look for any irritation or problems in the areas in the mouth that the appliance touches. They will also examine the denture or appliance itself, looking for any worn or broken areas.
References
1. "Geriatric Dentistry." American Dental Association.
2. "Geriatric Dentistry." MedlinePlus.
3. "Geriatric Dentistry: Meeting the Needs of an Aging Population." Journal of Dental Education.
4. "Geriatric Dentistry: A Review Article." Journal of Dental and Medical Sciences.
5. "Geriatric Dentistry: A Systematic Review of the Literature." Journal of the American Dental Association.
6. "Geriatric Dentistry: An Overview." Journal of Gerontology & Geriatric Research.
7. "Oral Health for Older Adults: A Guide for Family, Friends, and Caregivers." National Institute on Aging.
8. "Oral Health and Aging." Centers for Disease Control and Prevention.
9. "Geriatric Dentistry: Special Care Dentistry for Older Adults." Geriatrics and Gerontology International.
10. "Geriatric Dentistry: Changing Needs and Current Concepts." Journal of Aging Research & Clinical Practice.